HIPAA compliant AI therapy notes are clinical session documentation generated or assisted by artificial intelligence that adhere to all privacy, security, and data-handling requirements set forth by the Health Insurance Portability and Accountability Act (HIPAA). They help behavioral health clinics eliminate the burden of manual documentation while keeping client data protected and audit-ready.
For behavioral health clinicians, keeping up with therapy notes is one of the most time-consuming and compliance-sensitive parts of the job. AI-powered tools are changing that equation, but only when they’re built with HIPAA compliance at their core.
In this article, I will cover what HIPAA compliant AI therapy notes are, why they matter, the risks of non-compliant alternatives, real-world examples of compliant note formats, and how Alleva’s built-in AI tools make the entire process simpler and safer for behavioral health teams.
See how Alleva’s HIPAA compliant AI therapy notes work in practice. Book a free demo today.
What are HIPAA Compliant AI Therapy Notes?
HIPAA compliant AI therapy notes are clinical documentation records created with the assistance of artificial intelligence (such as ambient listening tools or AI writing assistants) that meet all HIPAA requirements for protecting Protected Health Information (PHI).
This means the AI system must operate under a signed Business Associate Agreement (BAA), store and transmit data through encrypted, HIPAA-compliant infrastructure, and ensure that no PHI is retained, shared, or exposed beyond what is clinically necessary.
The resulting notes are structured, accurate, and suitable for insurance submission, audits, and legal review. It should be a key feature of any EMR solution for behavioral health.
Stop letting documentation eat into your clinical time. Discover how Alleva’s compliant, task-based workflow can give your team hours back every week.
Why are HIPAA Compliant AI Therapy Notes Important?
HIPAA compliant AI therapy notes sit at the intersection of clinical quality, legal obligation, and operational efficiency. Here is why they matter for every behavioral health practice:
- Protects client privacy: HIPAA compliance ensures that sensitive mental health and substance use information is handled according to federal law, safeguarding clients from unauthorized disclosure.
- Reduces liability exposure: Compliant documentation practices protect clinicians and organizations from regulatory investigations, audits, and potential lawsuits stemming from improper PHI handling.
- Supports insurance reimbursement: Insurers require thorough, properly formatted notes to approve claims; AI-generated notes that meet clinical and compliance standards reduce claim denials and delays.
- Improves documentation accuracy: AI tools reduce the risk of human error, omissions, and inconsistencies that can create compliance gaps or complicate treatment continuity.
- Enables audit readiness: HIPAA compliant notes are structured and time-stamped in ways that satisfy both internal and external audits, reducing administrative scramble when reviews arise.
- Frees up clinician time: Automating compliant documentation means therapists spend fewer hours on paperwork and more hours providing direct client care, directly improving outcomes and reducing burnout.
- Ensures proper data governance: AI tools operating under a BAA are legally accountable for how they process PHI, giving practices a documented, enforceable layer of data protection.
Your clients deserve your full attention. Let Alleva handle the documentation. Book your personalized Alleva demo today and transform the way your team documents care.
Risks of Non-HIPAA Compliant AI Therapy Notes
Using AI tools that are not HIPAA compliant to generate or assist with therapy notes is not just a documentation shortcut, it is a federal compliance risk with serious financial and legal consequences.
Under the HIPAA Breach Notification Rule and the HIPAA Enforcement Rule, covered entities and their business associates are subject to civil monetary penalties ranging from $100 to $50,000 per violation, with annual caps reaching $1.9 million per violation category.
According to the U.S. Department of Health and Human Services Office for Civil Rights (OCR), which enforces HIPAA, penalties are tiered based on the level of culpability, meaning that willful neglect, such as knowingly using a non-compliant AI tool to handle PHI, can result in the highest penalty tier and even criminal referrals.
Beyond financial penalties, a reportable breach requires notifying affected individuals, the HHS Secretary, and in some cases the media, creating significant reputational harm for a behavioral health clinic. Non-compliant AI tools may also store session recordings or transcripts on unsecured servers, share data with third parties for model training without proper authorization, or fail to provide the audit trails required during an investigation.
For behavioral health organizations treating vulnerable populations, the stakes are especially high, a single breach can erode the trust that underpins the therapeutic relationship.
7 Examples of HIPAA Compliant AI Therapy Notes
The following examples illustrate what HIPAA compliant AI therapy notes look like across the most common formats used in behavioral health settings. Each example demonstrates how AI can generate structured, clinically sound documentation while protecting client privacy.
Example 1: SOAP Note — Individual Therapy Session
A SOAP note (Subjective, Objective, Assessment, Plan) is one of the most widely used formats in behavioral health documentation. When generated by a HIPAA compliant AI tool, the note captures what the client reported, what the clinician observed, a clinical assessment, and a clear treatment plan, all without retaining the underlying session audio.
AI-Generated SOAP Note Example:
Subjective: Client reports improved mood over the past week and states they have been practicing the breathing exercises discussed in the prior session. Client expressed mild anxiety about an upcoming family gathering but denied any depressive symptoms or suicidal ideation.
Objective: Client appeared calm and engaged throughout the session. Eye contact was appropriate. Speech was clear and goal-directed. No psychomotor abnormalities noted.
Assessment: Client demonstrates continued progress toward treatment goals related to anxiety management. Current coping strategies appear effective. No acute safety concerns.
Plan: Continue weekly individual therapy sessions. Introduce grounding techniques for use during the upcoming family event. Review anxiety log at next session.
Key Learnings:
- SOAP notes are ideal for tracking progress across sessions and are commonly required by payers
- AI tools should auto-populate consistent formatting to reduce clinician variance
- PHI such as the client’s name should only appear in designated, secured fields—not within the free-text note body
Pro tip: Configure your AI tool to flag incomplete SOAP sections before a note can be finalized, preventing submission gaps that trigger claim denials.
Example 2: DAP Note — Substance Use Counseling Session
A DAP note (Data, Assessment, Plan) is commonly used in substance use treatment settings for its streamlined format. HIPAA compliant AI can generate DAP notes in real time from session content, reducing documentation time significantly.
AI-Generated DAP Note Example:
Data: Client attended scheduled individual counseling session. Client reported completing seven days of sobriety and expressed pride in the milestone. Discussed triggers encountered at a social event over the weekend and strategies used to maintain sobriety. Client denied cravings in the past 48 hours.
Assessment: Client is making measurable progress toward sobriety goals. Demonstrated improved insight into personal triggers and applied relapse prevention strategies effectively. Risk for relapse appears low at this time.
Plan: Continue weekly counseling. Assign journaling exercise to track trigger patterns. Coordinate with group facilitator to reinforce peer support strategies.
Key Learnings:
- DAP notes are valued for their brevity and clarity, making them efficient for high-volume caseloads
- AI ambient tools can generate DAP notes from spoken session content within seconds of session close
- Ensure AI-generated notes are reviewed and signed by the licensed clinician to meet HIPAA and payer requirements
Pro tip: Use AI-generated DAP notes as a first draft and train your team to make targeted edits rather than starting from scratch, this cuts documentation time without sacrificing clinical quality.
Example 3: Utilization Review (UR) Note — Inpatient Behavioral Health
Utilization review notes are required to justify ongoing levels of care to insurance payers. These notes must be highly specific, clinically grounded, and formatted to meet payer criteria. AI tools trained on payer guidelines can generate UR notes that are more consistent and approval-ready than manually written versions.
AI-Generated UR Note Example:
Level of Care Justification: Client currently meets medical necessity criteria for continued residential treatment based on the following: persistent suicidal ideation with a recent attempt within the past 30 days, inability to maintain safety in a less restrictive environment, and need for 24-hour clinical monitoring and medication management.
Clinical Summary: Client has been in residential treatment for 14 days. Presenting diagnoses include Major Depressive Disorder, recurrent, severe, and Alcohol Use Disorder, moderate. Client is currently stabilizing on medication and engaging in daily individual and group therapy. Progress is incremental but consistent with the expected treatment trajectory.
Recommendation: Continued residential stay recommended for an additional 7 days pending clinical reassessment.
Key Learnings:
- UR notes must align precisely with diagnostic criteria and payer-specific language to avoid denials
- AI tools with built-in payer rule sets can significantly reduce UR denial rates
- HIPAA compliance is critical here because UR notes are often transmitted to insurance companies, ensuring secure, encrypted transmission is mandatory
Pro tip: Pair your AI UR note tool with an integrated insurance eligibility checker so level-of-care justifications are automatically calibrated to each payer’s requirements.
Example 4: Group Therapy Progress Note
Group therapy notes present a unique documentation challenge: clinicians must document each participant’s engagement and progress individually while keeping notes concise and compliant. AI tools can generate individualized group notes from a single session input.
AI-Generated Group Note Example (Individual Client Within Group):
Session Type: Group therapy, Cognitive Behavioral Therapy skills group (8 participants)
Client Participation: Client was present for the full 60-minute session. Actively participated in discussion around cognitive distortions, offering two personal examples. Demonstrated appropriate interpersonal boundaries and showed empathy toward peers. No disruptive behavior noted.
Clinical Observations: Client appears to be applying CBT concepts with increasing fluency. Affect was euthymic. No safety concerns observed during session.
Plan: Continue participation in weekly CBT group. Encourage client to practice thought records between sessions as discussed.
Key Learnings:
- Group notes must be individualized, a single blanket note for the whole group does not meet HIPAA or payer documentation standards
- AI tools that generate per-client group notes from a single session brief save significant time for group facilitators
- Session attendance and participation level should always be explicitly documented
Pro tip: Use a note template that prompts the AI to distinguish between active participation and passive attendance. Insurers often require evidence of meaningful engagement to justify reimbursement.
Example 5: Shift Handoff Note — Residential Treatment
In residential settings, shift handoff notes are critical for continuity of care. HIPAA compliant AI can generate structured handoff summaries that ensure the incoming team has everything they need without requiring manual note-writing between shifts.
AI-Generated Shift Handoff Note Example:
Shift Summary (3PM–11PM): Client expressed increased anxiety during the afternoon programming block and required 15 minutes of one-on-one support from the floor counselor. Medication administered as scheduled at 6PM with no adverse reactions reported. Client participated in dinner and evening group session. Declined recreation activity citing fatigue.
Safety Status: No safety concerns during this shift. Client denied SI/HI at last check-in at 10:30PM.
Handoff Items for Incoming Shift: Monitor client’s anxiety levels during morning programming. Client has a scheduled phone call with family at 9AM, coordinate with counselor to provide support as needed. Medication due at 7AM per MAR.
Key Learnings:
- Shift handoff notes must be time-stamped, attributed to the documenting staff member, and stored securely within the EHR
- AI-generated handoff notes reduce the risk of verbal-only shift transitions where critical details can be lost
- Any safety-related observations from the prior shift should be prominently flagged at the top of the handoff note
Pro tip: Integrate shift handoff notes directly into your EHR’s task management system so incoming staff receive real-time alerts on flagged clients before their shift begins.
Example 6: Treatment Plan Progress Note
Treatment plan progress notes document a client’s movement toward specific therapeutic goals and are typically required at regular intervals (e.g., every 30 days) to satisfy accreditation and payer requirements. AI tools can cross-reference existing treatment plan goals and auto-populate progress indicators.
AI-Generated Treatment Plan Progress Note Example:
Review Period: 30-day treatment plan review
Goal 1 — Reduce anxiety symptoms: Client has made moderate progress. Reports a reduction in panic episodes from 4–5 per week to 1–2 per week. Continues to practice diaphragmatic breathing daily. Goal remains active.
Goal 2 — Improve social functioning: Client has made significant progress. Successfully attended two community social events during the review period and reported positive experiences. Goal on track for completion by next review.
Goal 3 — Medication adherence: Client has maintained 100% medication adherence during the review period. Goal met. Recommend transitioning to maintenance monitoring.
Updated Plan: Revise Goal 3 to reflect maintenance phase. Add new goal focused on relapse prevention education. Next review scheduled in 30 days.
Key Learnings:
- Treatment plan progress notes should map directly to the original goals documented at intake, AI tools that link notes to the treatment plan template ensure consistency
- Rating goal progress (e.g., minimal, moderate, significant) helps payers evaluate medical necessity for continued care
- Notes should always reflect the clinician’s clinical judgment, even when AI-generated drafts are used as a starting point
Pro tip: Set automated reminders in your EHR to flag when a 30-day treatment plan review is approaching so clinicians can review the AI draft, make edits, and sign on time.
Example 7: Telehealth Session Note
As telehealth becomes a permanent fixture in behavioral health, documentation must reflect the unique characteristics of virtual sessions, including platform used, technical issues, and confirmation of client location for interstate licensing and billing compliance. HIPAA compliant AI tools built for telehealth can capture these details automatically.
AI-Generated Telehealth Session Note Example:
Session Format: Individual telehealth session conducted via HIPAA-compliant video platform. Client connected from home (confirmed within licensed state). No significant technical disruptions. Session duration: 50 minutes.
Session Summary: Client presented as calm and engaged. Discussed ongoing challenges with work-related stress and explored cognitive reframing strategies. Client expressed interest in trying mindfulness-based techniques and was provided with two guided exercises to practice before the next session.
Clinical Observations: Client’s affect appeared appropriate via video. No concerning behavioral indicators noted. Client denied SI/HI.
Plan: Continue weekly telehealth sessions. Follow up on mindfulness practice at next session. Client confirmed next appointment.
Key Learnings:
- Telehealth notes must document platform compliance, client location, and session duration to satisfy both HIPAA and billing requirements
- AI tools integrated with telehealth platforms can auto-populate session metadata, reducing manual entry errors
- Clinicians should confirm client identity and location verbally at the start of each telehealth session and ensure the AI note captures this confirmation
Pro tip: Choose an AI documentation tool that is natively integrated with your telehealth platform so session metadata flows directly into the note without requiring manual input from the clinician.
How To: Using Alleva’s HIPAA Compliant AI Therapy Notes
Alleva is a behavioral health EHR platform built specifically for mental health and substance use treatment, and its HIPAA compliant AI therapy notes are a direct reflection of that focus. Every documentation feature is designed to meet the privacy, security, and clinical standards that behavioral health providers actually face.
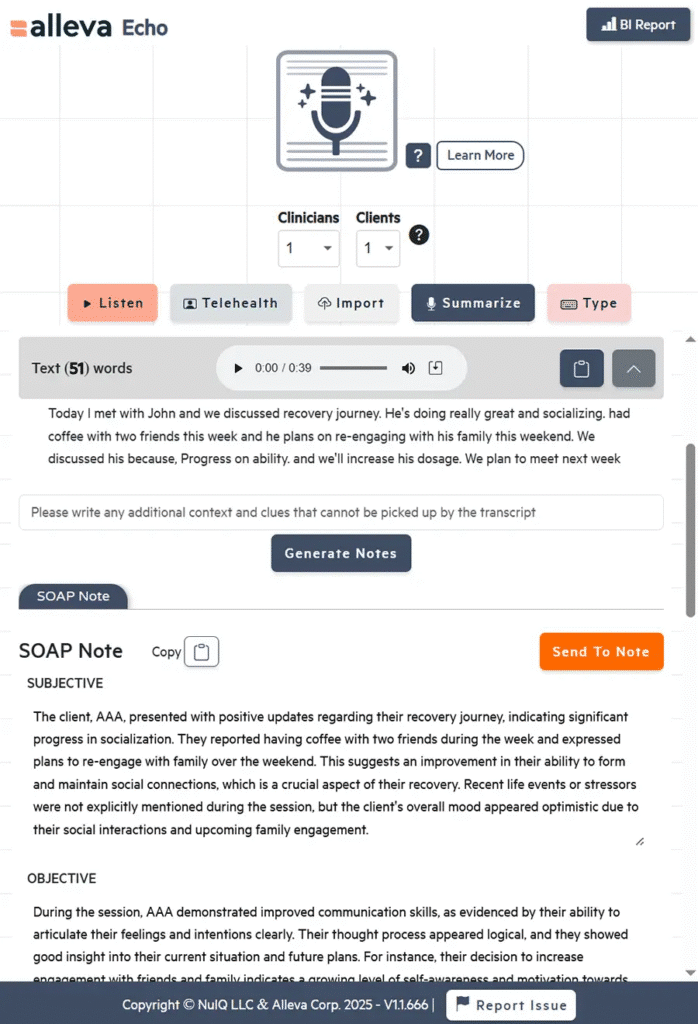
Echo and TravisAI: Two AI Tools, One Integrated Platform
Alleva’s HIPAA compliant AI therapy notes are powered by two built-in tools: Echo and TravisAI. Echo is Alleva’s ambient AI that listens to sessions and generates structured, audit-ready notes in real time (supporting DAP, SOAP, UR, and more) without ever saving a recording.
Only secure, compliant notes remain, keeping PHI protected at every step. TravisAI complements Echo by serving as an in-platform AI assistant that answers documentation questions and guides clinicians through compliance workflows on the spot.
Ready to put Echo and TravisAI to work for your team? Schedule a personalized Alleva demo and see both tools in action.
Smarter, Compliant Notes, Built Into Your Workflow
Alleva’s HIPAA compliant AI therapy notes don’t exist in isolation, they’re embedded into a task-based workflow that automates note generation, schedules documentation based on calendar events and clinical needs, and reduces compliance risk across the board. Customizable templates ensure every note meets payer and regulatory standards, while intuitive task lists keep clinicians on track so nothing falls through the cracks.
HIPAA Compliant Notes Across Every Level of Care
Whether your program is intensive outpatient, partial hospitalization, or 24/7 residential, Alleva generates HIPAA compliant AI therapy notes at every level. Residential teams can document shift handoffs, progress notes, and safety observations in one system, with every entry captured, compliant, and accessible to the right staff at the right time.
Secure Infrastructure That Connects Notes to Billing
Alleva’s HIPAA-compliant infrastructure ensures that every AI-generated therapy note is stored and transmitted securely, and syncs directly with billing, scheduling, and outcomes tracking. Because notes feed seamlessly into claim submission, your team avoids the manual re-entry errors that create both compliance gaps and reimbursement delays. The result is documentation that is not only audit-ready, but revenue-ready too.
A Full EHR Built Around Compliant Documentation
Alleva’s HIPAA compliant AI therapy notes are part of a full Electronic Health Record (EHR) system that goes beyond what a standard EMR offers. Where EMRs focus on clinical documentation within a single setting, Alleva’s EHR connects AI-generated notes to the entire continuum of care (admissions, treatment planning, e-prescribing, outcomes tracking, billing, and cross-team coordination) all within a compliant, behavioral health-specific platform.
HIPAA Compliant AI Therapy Notes Made Simple
HIPAA compliant AI therapy notes are an operational reality for behavioral health clinics that want to protect their clients, satisfy payers, and give their clinical teams back the time they deserve. The difference between a compliant AI documentation tool and a non-compliant one is not just a matter of features; it is a matter of legal exposure, client trust, and the integrity of your entire clinical operation.
Choosing a platform like Alleva, which has built HIPAA compliance into every layer of its AI documentation tools, means your team can focus on what they do best: delivering exceptional care.
Ready to see what HIPAA compliant AI therapy notes look like in action for your team? Book a personalized demo with Alleva today and discover how Echo, TravisAI, and Alleva’s full EHR platform can transform your documentation workflow, from the first session note to the final billing claim.