Alleva Billing
Your Revenue Cycle, Simplified
Alleva Billing connects your clinical and financial workflows in one place,
from charge capture to claim submission and ERA posting.
Stay compliant, reduce denials, and get paid faster.
from charge capture to claim submission and ERA posting.
Stay compliant, reduce denials, and get paid faster.
Built-In. Automated. Designed for Behavioral Health.

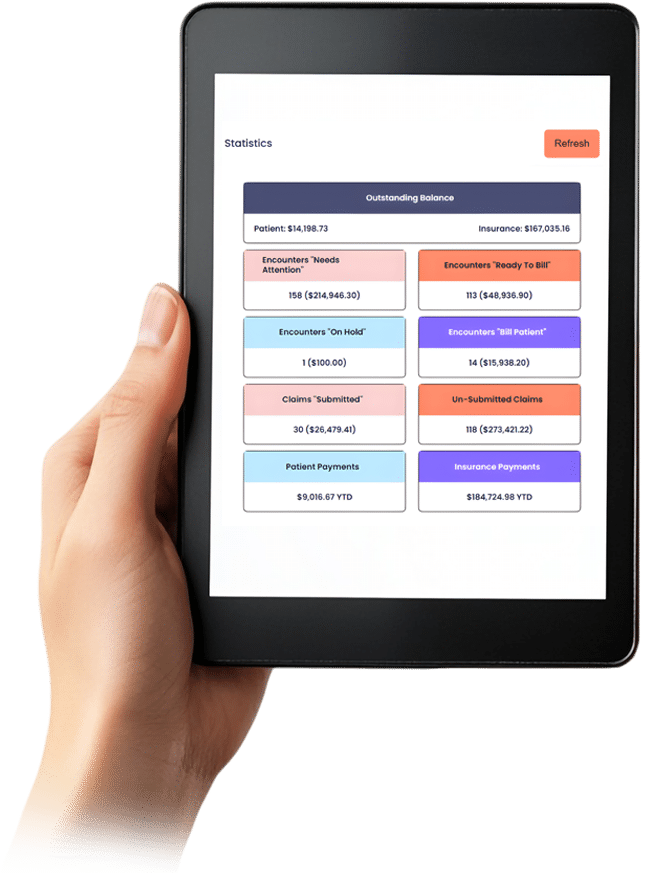
Core Billing
Platform
With automation and real-time tracking, Alleva Billing streamlines claims, accelerates reimbursements, and gives finance teams full visibility into revenue.
Control and Accuracy
in Billing Workflow
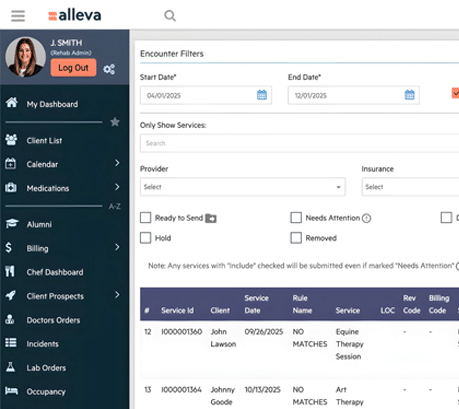
Encounter Transmission Table (ETT)
ETT ensures precision from encounter to claim, allowing real-time editing and review before submission.
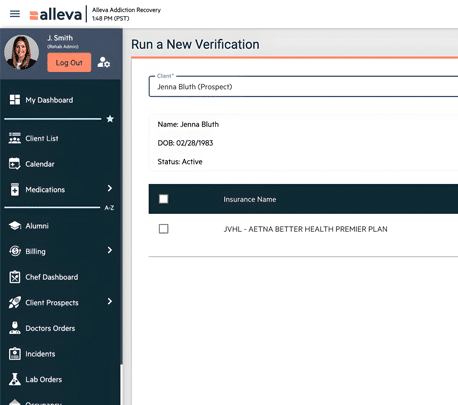
Instant VOBs
Integrated instant VOBs confirm insurance eligibility within seconds — reducing intake delays and improving financial accuracy all within the platform.
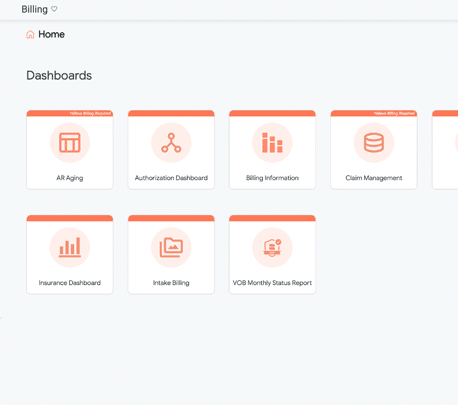
Automation & Intelligence
Automate claim creation, prevent rejections, and eliminate manual posting — so teams can focus on patient care, not paperwork.
Trust
SHOW RESULTS AND RELIABILITY.
Alleva Billing averages a 9% denial rate compared to the industry 30% end-to-end.

See Alleva Billing in Action
Clarity and
Confidence.
Simplify your billing. Strengthen your revenue.
Empower your care.
Empower your care.

