Looking for help on how to choose an ehr system for your behavioral health practice? Choosing an EHR system for behavioral health is a procurement decision that determines how your clinical, admissions, and billing teams operate, and how much time your clinicians actually spend with clients versus documentation.
Behavioral health organizations navigating this decision face real stakes. An EHR that doesn’t fit your workflows creates documentation burden, compliance risk, and staff frustration. One that fits well can reduce administrative time, support cleaner billing, and free clinicians to focus on care.
Explore whether Alleva’s purpose-built behavioral health EHR fits your organization.
This guide walks through the full evaluation process, from mapping your workflows to negotiating your contract, including how emerging AI documentation tools are reshaping what behavioral health organizations should require from a vendor.
Assess Your Clinical Workflows Before You Shop
Behavioral health teams navigating complex workflows should begin by mapping how care actually happens today, not how it is supposed to happen.
Document intake flows, assessments, group and individual session documentation, medication management, care coordination, consent and release workflows, and billing handoffs. Include representatives from clinical, admissions, billing, IT, and compliance to capture handoffs and exceptions.
Practical steps:
- Shadow clinicians and collect sample notes and data exports during a time-boxed discovery phase.
- Measure current documentation time per encounter and identify your most-used templates.
- Audit data quality: required-field completion rates, free-text frequency, and common coding problems.
- Flag daily integrations needed: labs, pharmacies, payer eligibility, and state reporting portals.
Documenting these details helps you prioritize which workflows must be preserved, which can be improved, and which require structured change management during transition.
Key EHR Features for Addiction and Mental Health Programs
Focus on features that reduce clinician burden and support the regulatory requirements specific to SUD and mental health care. Look for built-in or configurable tools for treatment planning, group therapy documentation, screening and outcome measures, and medication-assisted treatment (MAT) workflows.
Operational and clinical features to prioritize:
- Structured treatment plans with goals, objectives, and progress tracking.
- Group notes and attendance tracking with configurable templates.
- ASAM Criteria integration for addiction treatment programs.
- Controlled-substance prescribing workflows and PDMP integration.
- Behavioral health screening and outcome measure tracking (PHQ-9, GAD-7, CAGE-AID) in support of measurement-based care (MBC) frameworks.
- Integrated telehealth documentation for individual, group, and family sessions.
- Client and family portal for scheduling, reminders, and secure messaging.
- Integrated CRM and admissions pipeline to reduce duplicate data entry.
- Billing codes and payer rules tuned for behavioral health, with built-in RCM visibility.
Features that reflect daily clinical practice reduce training time and preserve care continuity while improving financial workflows.
Evaluating AI Documentation Capabilities: A New Essential Criterion
AI-powered documentation has moved from early adoption to a standard EHR evaluation criterion in 2025–2026. Behavioral health organizations should now assess ambient AI capabilities as part of any EHR selection process.
What ambient AI documentation means in practice:
Ambient AI tools listen to clinical sessions, whether in-person or via telehealth, and generate structured, audit-ready session notes in real time. These notes are reviewed and approved by the clinician before entering the chart. The most clinically relevant formats for behavioral health include DAP, SOAP, BIRP, and group note structures.
Why this matters for your evaluation:
Research published in JAMA Network Open (2025) found that clinicians using ambient AI spent measurably less time in the EHR and reported reduced cognitive load and improved satisfaction. For behavioral health, where “pajama time”, documentation completed after hours, is a well-documented contributor to clinician burnout, ambient AI is a meaningful clinical workflow tool, not just a productivity feature.
Key questions to ask vendors about AI documentation:
- Is the ambient AI tool native to the EHR, or a third-party add-on requiring copy-paste?
- Does the AI support behavioral health-specific note types (DAP, SOAP, BIRP, group notes)?
- Is the recording discarded after note generation, or stored? (HIPAA and 42 CFR Part 2 implications apply.)
- Does the vendor provide a signed BAA covering their AI tools specifically?
- Does your state require patient disclosure when AI is used in clinical documentation? (California AB 3030, effective January 2025, and Texas’s Responsible AI Governance Act, effective January 2026, are examples.)
An EHR with a native, HIPAA-compliant ambient AI tool built for behavioral health note types offers a meaningfully different workflow than a system that relies on a third-party scribe integration.
Verifying Interoperability with Labs, Pharmacies, and Hospitals
Vendors may state broad interoperability, but verification requires technical evidence and real-world references. Request interface specifications, transport protocols (HL7 v2, HL7 FHIR, X12), and whether the vendor uses certified intermediaries or direct interfaces.
Practical verification steps:
- Request test endpoints or a sandbox to run sample orders, results, and FHIR resources.
- Ask for interface documentation and SLAs for message delivery and error handling.
- Obtain customer references using the same integration types you need; ask about data accuracy and downtime.
- Confirm patient matching, identifier mapping, and reconciliation procedures for discrepant results.
A clear interoperability plan reduces go-live risk and supports participation in the broader clinical ecosystem. Understanding HL7 standards and behavioral health interoperability helps organizations ask the right technical questions during vendor evaluations.
Compliance, Privacy, and 42 CFR Part 2
Behavioral health data is governed by both HIPAA and, for substance use disorder programs, 42 CFR Part 2, a stricter federal confidentiality regulation that restricts disclosure of SUD treatment records more narrowly than standard HIPAA rules.
Evaluate vendors on both frameworks explicitly. Request:
- A Business Associate Agreement (BAA) covering all modules, including AI tools and third-party integrations.
- Confirmation that the system supports 42 CFR Part 2-compliant consent workflows if your program treats SUD clients.
- Encryption at rest and in transit, role-based access controls, audit logging, and multi-factor authentication.
- SOC 2 attestation, penetration testing schedules, and breach notification procedures.
- Data residency, backup, and retention policies.
A strong security posture and clear contractual commitments protect PHI and reduce operational risk. These commitments should be reflected in your RFP and contract.
Licensing, Hosting, and Total Cost of Ownership
Understand the difference between subscription (SaaS) and one-time licensing models and how they affect your total cost of ownership.
Tradeoffs to consider:
- SaaS: Predictable operating expense; vendor-managed updates; lower internal IT burden. Per-user or per-facility pricing is common.
- One-time license: Larger upfront capital expense; more internal IT responsibility for hosting and upgrades.
- Cloud-based multi-tenant SaaS is typically the most scalable and lowest-burden option for growing or multi-location behavioral health organizations.
When calculating TCO, include software fees, hardware, implementation, data migration, training, ongoing support, and exit costs. These calculations often shift the apparent cost advantage of lower-priced vendors.
Building an RFP and Vendor Evaluation Matrix
An effective RFP combines functional requirements, technical and security requirements, implementation expectations, and commercial terms. Use a weighted vendor evaluation matrix to score vendors across categories objectively.
RFP checklist:
- Functional: clinical documentation, MAT workflows, ASAM integration, group notes, telehealth, AI documentation, CRM and RCM.
- Technical: APIs, FHIR/SMART support, interface specifications, 42 CFR Part 2 support.
- Security: BAA, encryption, audit logging, SOC 2, 42 CFR Part 2 compliance.
- Implementation: data migration approach, training plan, timeline, and resource commitments.
- Commercial: pricing model, support SLAs, escalation terms, and exit costs.
A transparent scoring matrix moves the conversation from marketing claims to verifiable capabilities. It also gives internal stakeholders a structured basis for comparison.
Usability Testing Before You Purchase
Formally testing usability before committing reduces clinician frustration and adoption delays. Run role-based workflow demos, scripted clinical scenarios, and summative usability tests.
Testing framework:
- Observe clinicians performing core tasks using realistic patient scenarios.
- Include intake staff and billing users to validate cross-team workflows.
- Measure time on task, error types, and completion rates for key tasks.
- Run a small pilot group to validate training plans and identify configuration issues.
Testing results should directly inform configuration, training scope, and your final vendor decision.
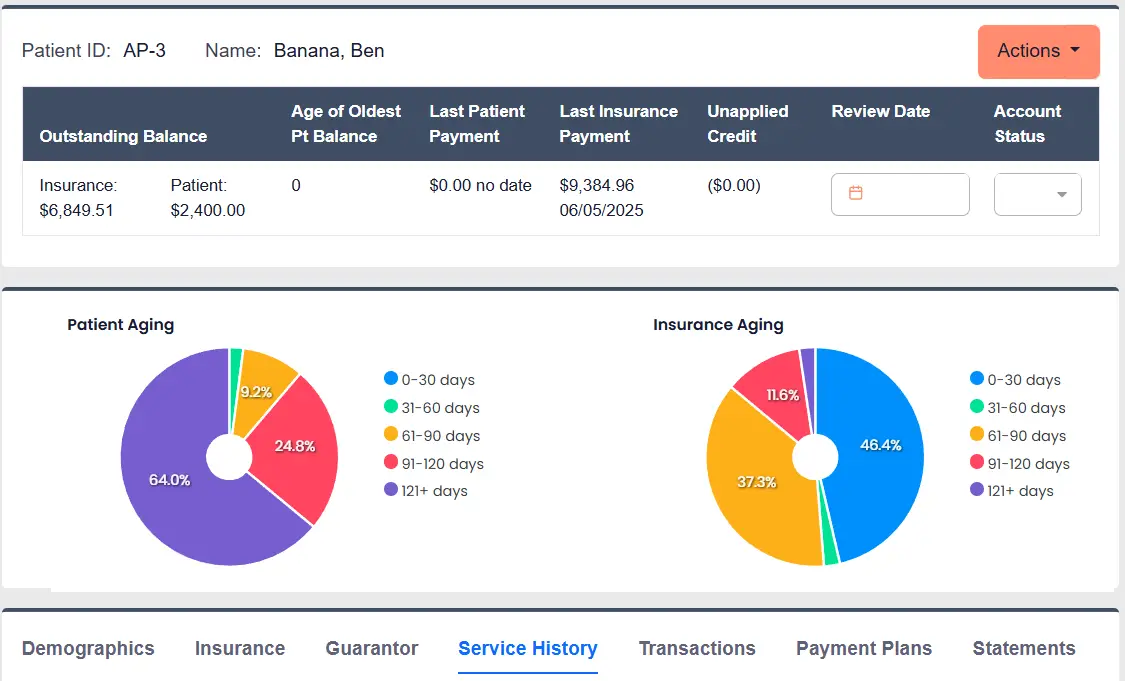
KPIs to Track in the First 6–12 Months
Monitor KPIs across adoption, documentation efficiency, financial performance, and clinician experience.
Recommended metrics:
- Adoption: percentage of clinicians using the system daily; documentation completion rates.
- Documentation efficiency: average time per encounter; after-hours documentation volume.
- Financial: claim denial rate; days in accounts receivable; revenue capture for billable services.
- Support: volume and severity of support tickets; system uptime; mean time to resolve.
- Clinician experience: satisfaction surveys; perceived administrative burden.
- Patient access: referral-to-first-appointment time; intake completion rates.
Review these KPIs regularly with your vendor and internal stakeholders to adjust workflows, training, and configuration.
Schedule a Demo to Explore Whether Alleva Fits Your Needs
If your organization is working to reduce documentation burden, improve care coordination, and simplify behavioral health billing, scheduling a demo is the most practical next step.
FAQs: Choosing a Behavioral Health EHR
How do we assess workflows and data quality before choosing an EHR?
Shadow clinicians and map end-to-end workflows for intake, assessments, treatment planning, medication management, group documentation, and billing. Audit required-field completion rates, documentation time per encounter, and common coding problems. Include stakeholders from clinical, admissions, billing, compliance, and IT.
Which features matter most for addiction and mental health programs?
Prioritize structured treatment planning, group note templates, ASAM Criteria integration, MAT workflows with PDMP access, screening and outcome measure tracking (PHQ-9, GAD-7), telehealth documentation, client portals, and integrated RCM.
How do we verify interoperability claims?
Request technical interface documentation (HL7 v2, FHIR, X12), test endpoints, and customer references using the same integration types. Confirm patient matching procedures, error handling, and SLAs.
What should we know about 42 CFR Part 2?
42 CFR Part 2 is a federal regulation governing SUD treatment records that is stricter than HIPAA. If you treat substance use disorder clients, confirm the EHR supports 42 CFR Part 2-compliant consent and disclosure workflows, and that the vendor’s BAA explicitly covers this obligation.
How do we evaluate AI documentation features?
Ask whether ambient AI is native to the EHR or a third-party add-on, which behavioral health note types it supports, how audio is handled after note generation, and whether the vendor provides a BAA that covers AI tools. Also verify whether your state has specific patient disclosure requirements for AI use.
What contract terms matter most?
A signed BAA, data portability and export rights with defined timelines, exit assistance, SLAs, and pricing escalation terms. Clarify data ownership, backup, retention, and breach notification responsibilities.
Choose a Behavioral Health EHR that best fits your needs
When you’re looking for a behavioral health EHR, you should first identify your goals and needs. It doesn’t matter how great a mental health EHR software is if it doesn’t do what you need it to. Once you’ve established this, look at your current process and find an EHR that keeps what’s currently working for you.
Next, assign priority to the pains and items you want to keep in order of importance. Then make a list of potential EHR vendors and get references on them. The best way to conduct an EHR search is to make it thorough. Then, get a demo! Most, if not all, EHR vendors provide a free demo. If they don’t, you probably shouldn’t consider that vendor. You can schedule a no-hassel demo with us here.
Check your current contract to ensure it doesn’t have any clauses preventing you from leaving without sufficient notice. If you’re able to leave your current contract, don’t do so until you know the new vendor is a good fit technically and culturally. If it is going to save you time and give you peace of mind, it will be worth the switch.

